This informal CPD article, ‘Calming the Nervous System: How Vagus Nerve Stimulation Can Help Ease Anxiety’, was provided by Parasym, a neurotechnology company focused on developing innovative neuromodulation treatments to improve quality of life.
Anxiety disorders are among the most common mental health conditions. Between 2022 to 2023, 37% of women and 30% of men in the UK reported to have experienced high levels of anxiety.¹ These symptoms often lead to distress and can interfere with daily functioning.² While medications and therapy remain the foundation of treatment, an emerging non-invasive approach known as vagus nerve stimulation (VNS) is gaining attention as a promising alternative for symptom relief.
Understanding the Vagus Nerve’s Role in Anxiety
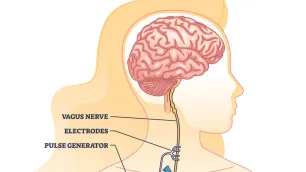
The vagus nerve is critical for the body’s “rest and digest” system and regulates key functions such as heart rate, digestion, and mood.³ When the vagal tone is low, the body is more likely to stay in a state of heightened alert, which can worsen anxiety. Stimulating the vagus nerve may restore balance to the nervous system, thus reducing the fight-or-flight response and promoting relaxation.
Studies have shown that individuals with anxiety often exhibit signs of reduced vagal tone, where their parasympathetic (calming) activity is low with an overactive stress response system.³ This imbalance doesn’t just affect mood, it also impacts inflammation and other bodily systems. Boosting vagus nerve activity through stimulation may help shift the body toward a calmer, more resilient state.
Invasive VNS has been approved by the FDA since the late 1990s for conditions like epilepsy and treatment-resistant depression, but its widespread use has been limited by the need for surgical implantation, associated risks, and high costs. In contrast, transcutaneous auricular vagus nerve stimulation (taVNS) emerged as a non-invasive, safer, and more accessible alternative.⁴
What the Evidence Suggests
TaVNS stimulates the vagus nerve by sending mild electrical impulses to the outer ear where the vagus nerve is accessible. Recent studies suggest that this can significantly reduce anxiety. In one clinical trial, healthy university students who received taVNS reported lower anxiety and muscle tension compared to a control group.⁵
Bretherton et al. found that using taVNS daily improved mood and heart rate variability, an important measure of the state of our nervous system in adults over 55.⁶ This supports the idea that even short-term stimulation can positively impact stress levels and emotional resilience.
In addition, a 2025 review also showed that taVNS appears effective not only in healthy individuals but also in those with anxiety disorders and PTSD.⁷ Researchers found improvements in both emotional regulation and brain network activity related to stress control.
Unlike lifestyle-based vagus nerve stimulation methods such as meditation, deep breathing, cold exposure, or humming, taVNS devices do not require attention, training, or habit-building. They can be used passively while performing other activities.
How VNS Works in the Brain
VNS appears to influence areas of the brain that regulate emotions, including the amygdala and prefrontal cortex.⁸ It also affects important brain chemicals such as serotonin and GABA, both of which are involved in mood and anxiety. Brain imaging studies show that taVNS can alter how different brain regions connect and communicate, particularly those involved in emotional control and stress responses.⁷
VNS may also quiet down the brain’s “default mode network,” a neurological system that tends to be overactive in people who ruminate or worry excessively.⁷ This could help explain why users of taVNS often report feeling calmer and more focused.
Looking Ahead: Clinical Promise
What makes taVNS appealing is that it’s non-invasive and user-friendly. It offers an option for people who don’t respond well to medication or want to avoid side effects from pharmacotherapies. With its strong safety profile, taVNS is increasingly being considered as an addition to traditional anxiety treatments.
Early clinical trials, such as one involving people with borderline personality disorder, suggest that taVNS may help with emotional regulation even in complex mental health conditions.⁸
As wearable health tech evolves, taVNS devices are becoming more accessible for home use. Devices are currently being studied across various health conditions, including mental health, and early results show high tolerability and positive feedback.
For now, it’s important that clinicians stay informed about this promising tool as part of a whole-person approach to mental health care.
We hope this article was helpful. For more information from Parasym, please visit their CPD Member Directory page. Alternatively, you can go to the CPD Industry Hubs for more articles, courses and events relevant to your Continuing Professional Development requirements.
References:
- Mental Health Foundation. Anxiety Statistics. https://www.mentalhealth.org.uk/explore-mental-health/statistics/anxiety-statistics
- Baxter AJ, Scott KM, Vos T, Whiteford HA. Global prevalence of anxiety disorders: a systematic review and meta-regression. Psychol Med. 2013;43(5):897-910. https://doi.org/10.1017/S003329171200147X
- Breit S, Kupferberg A, Rogler G, Hasler G. Vagus nerve as modulator of the brain–gut axis in psychiatric and inflammatory disorders. Front Psychiatry. 2018;9:44. https://doi.org/10.3389/fpsyt.2018.00044
- Yap JYY, Keatch C, Lambert E, Woods W, Stoddart PR. Critical review of transcutaneous vagus nerve stimulation: challenges for translation to clinical practice. Front Neurosci. 2020;14:284. https://doi.org/10.3389/fnins.2020.00284
- Ferreira LMA, Brites R, Fraião G, et al. Transcutaneous auricular vagus nerve stimulation modulates masseter muscle activity, pain perception, and anxiety levels in university students: a double-blind, randomized, controlled clinical trial. Front Integr Neurosci. 2024;18:1422312. https://doi.org/10.3389/fnint.2024.1422312
- Bretherton B, Atkinson L, Murray A, Clancy J, Deuchars S, Deuchars J. Effects of transcutaneous vagus nerve stimulation in individuals aged 55 years or above: potential benefits of daily stimulation. Aging (Albany NY). 2019;11(14):4836-4857. https://doi.org/10.18632/aging.102074
- Croft JR, LaMacchia ZM, Alderete JF, et al. Transcutaneous auricular vagus nerve stimulation: efficacy, applications, and challenges in mood disorders and autonomic regulation. Mil Med. 2025. https://doi.org/10.1093/milmed/usaf063
- Guerriero G, Liljedahl SI, Carlsen HK, et al. Transcutaneous auricular vagus nerve stimulation to acutely reduce emotional vulnerability and improve emotional regulation in borderline personality disorder (tVNS-BPD): study protocol for a randomized, single-blind, sham-controlled trial. Trials. 2024;25(1):397. https://doi.org/10.1186/s13063-024-08230-6


