
This informal CPD article, ‘The Microbiota-Gut-Brain Axis and Mood’, was provided by ADM Protexin, who are dedicated to producing innovative, research based live bacteria (Probiotic) products for the veterinary, human, agriculture and equine healthcare markets.
What is Low Mood?
Low mood is categorised as feelings of sadness, tiredness, low self-esteem or frustration/anger. These feelings are often transient and will lift after a few days or weeks.1 Low mood that persists longer-term, may indicate a more serious underlying problem – such as depression – and individuals should seek advice from an appropriate health care practitioner.
Depression can be diagnosed using two main classification systems, but broadly speaking the content of the two systems is very similar: there are core symptoms, such as low mood and anhedonia (and inability to take pleasure in things), fatigue and impaired concentration; and there are biological symptoms e.g. insomnia, changes in appetite or reduced libido.2 Such symptoms may interfere with an individual’s ability to work and maintain personal relationships. Whilst low mood is a common symptom of depression; without the presence of other factors, the criteria for a clinical diagnosis of depression may not be met.
For individuals with a clinical diagnosis involving low mood (such as depression), they may be offered a combination of therapies, including cognitive behavioural therapy, counselling and medication.3 Unfortunately, a substantial number of people experiencing depression do not respond to conventional treatment, whilst medical costs often increase and health-related quality of life decreases.4 Therefore research has highlighted a need for improved therapies in this patient group.4
Theoretical Mechanisms of Action
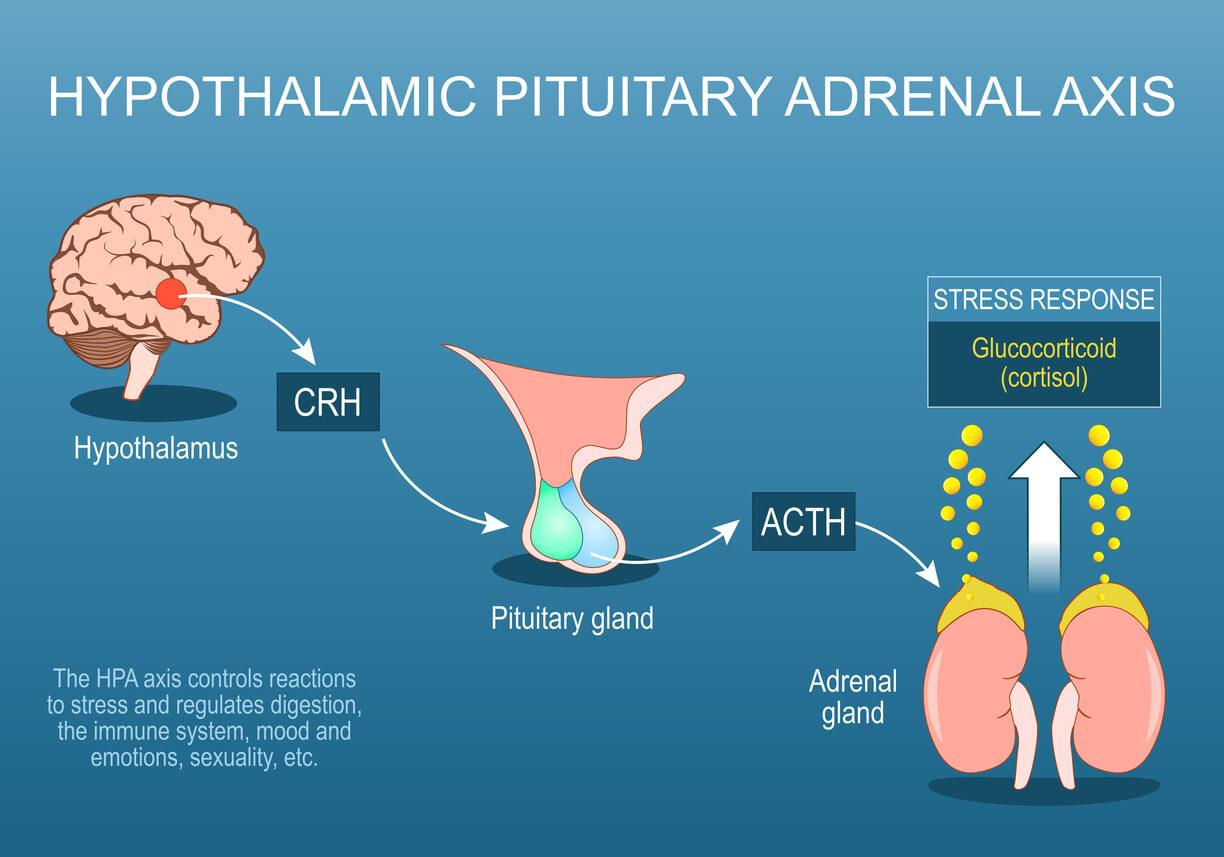
The reason for an altered mood state will vary between individuals, context and scenario,5 and multiple mechanisms may play a role. However, one prominent system that has been associated with low mood is the activation of the hypothalamic-pituitary-adrenal (HPA) axis.5
The biological consequences of chronic stress on the body is a concept known as allostatic load.6 This term emphasises the cascading relationships (beginning in early life), between environmental factors and genetic predispositions that may lead to distinct differences in susceptibility to altered stress responses and ill-health.6 Stress may be categorised as ‘good’, ‘tolerable’ or ‘toxic’ stress, with the latter two predisposing an individual to a degree of allostatic load.7,8
- Good stress – involves taking part in an activity that is perceived as stressful, but provides a reward when completed (such as a job interview or public speaking). Stress mediators promote adaptation during the event and are then turned off when the task is complete.
- Tolerable stress – when something bad happens (such as losing a job or ending a relationship), but personal resources and/or support systems allow the individual to ‘weather the storm’ and become resilient. Stress responses may fluctuate on and off to promote adaptation.
- Toxic stress – also when something bad happens (as in tolerable stress), but the individual lacks resources or support systems. This scenario may result in a reduced sense of control and potentially leads to chronic physiological dysregulation.
Allostatic load may contribute to the dysregulation of the HPA axis and disturbances in mood.8,9 Activation of the HPA axis may initially be influenced by prenatal environmental stressors, as well as further psychosocial influences such as adverse childhood events. It has been suggested that these factors may programme the HPA axis, by epigenetics to function at a higher ‘set point’.10–12 Consequently, this lowered threshold for stress resilience, combined with chronic (or toxic) stress, could form triggers to dysregulated mood.
Mood and the Gut
Communication between the gut and the brain is proposed to exist via a variety of pathways; including direct nerve supply, enteroendocrine cells, microbial-associated molecular patterns (MAMPS) and direct synthesis of some neurotransmitters and neuromodulators.13 Evidence suggests a correlation between digestive symptoms and mood. One study found that patients with irritable bowel syndrome (IBS) of all sub-types had more frequent and severe depressive symptoms compared to healthy controls.14 Significant increases in intestinal inflammatory markers, anti-bodies, zonulin and lipopolysaccharides have also been correlated with severe mental illness compared to controls.15 The markers assessed were linked with dysbiosis, highlighting the role the microbiome may play in some mood disorders. Whilst an important distinction between clinical diagnoses and low mood must be drawn, evidence suggests that gut dysbiosis may coexist with symptoms seen in individuals with low mood and depression - and this provides a rationale for future investigations into modulation of the gut microbiome in mood disorders.15
The Use of Live Bacteria Supplements in Low Mood
Live bacteria have the potential ability to reduce intestinal inflammation and lower stress hormones.16–18 Supplementation may also be helpful through the action of bacteria-derived metabolites. Short-chain fatty acids (SCFAs) are mainly produced by bacterial fermentation of dietary fibres.19 They may help to reduce intestinal inflammation, support gut barrier defences and communicate with immune cells.19 Evidence is now suggesting that SCFAs may also play a role in depressive-like behaviours.20
Conclusion
As research of the microbiota-gut-brain axis develops, the focus now is translating findings from preclinical studies to human clinical trials. The use of live bacteria supplementation in the management of low-mood warrants consideration based on the proposed mechanisms of action; including synthesis of neurotransmitters and neuromodulators, tryptophan metabolism, supporting gut barrier defences and communication with the immune system and inflammatory response.21–23 The determinants of mood are complex and subjective, therefore it is important to appreciate a personalised approach to therapies. This may include a combination of supplements, diet and lifestyle changes, with the support of an appropriately qualified practitioner.
We hope this article was helpful. For more information from ADM Protexin, please visit their CPD Member Directory page. Alternatively, you can go to the CPD Industry Hubs for more articles, courses and events relevant to your Continuing Professional Development requirements.
References:
1 Low mood and depression | NHS inform. https://www.nhsinform.scot/healthy-living/mental-wellbeing/low-mood-and-depression/low-mood-and-depression (accessed March 3, 2021).
2 Context | Depression in adults: recognition and management | Guidance | NICE. National Institute for Health and Care Excellence. 2009. https://www.nice.org.uk/guidance/cg90/chapter/Context#care-of-all-people-with-depression (accessed March 3, 2021).
3 Clinical depression - Treatment - NHS. 2019. https://www.nhs.uk/conditions/clinical-depression/treatment/ (accessed March 5, 2021).
4 Johnston KM, Powell LC, Anderson IM, Szabo S, Cline S. The burden of treatment-resistant depression: A systematic review of the economic and quality of life literature. Journal of Affective Disorders 2019; 242: 195–210.
5 Malhi GS, Mann JJ. Depression. The Lancet 2018; 392: 2299–312.
6 McEwen BS, Stellar E. Stress and the Individual: Mechanisms Leading to Disease. Archives of Internal Medicine 1993; 153: 2093–101.
7 Shonkoff JP, Julius Richmond FAMRI Professor of Child Health CB, Thomas Boyce W, et al. Council Members Contributing Members National Scientific Council on the Developing Child National Forum on Early Childhood Program Evaluation. 2007.
8 Guidi J, Lucente M, Sonino N, Fava GA. Standard Review Article Allostatic Load and Its Impact on Health: A Systematic Review. 2019. DOI:10.1159/000510696.
9 Rao R, Androulakis IP. Allostatic adaptation and personalized physiological trade-offs in the circadian regulation of the HPA axis: A mathematical modeling approach. Scientific reports 2019; 9: 11212.
10 Scheinost D, Sinha R, Cross SN, et al. Does prenatal stress alter the developing connectome? Pediatric Research 2017; 81: 214–26.
11 Zhong X, Ming Q, Dong D, et al. Childhood Maltreatment Experience Influences Neural Response to Psychosocial Stress in Adults: An fMRI Study. Frontiers in Psychology 2020; 10: 2961.
12 Karin O, Raz M, Tendler A, et al. A new model for the HPA axis explains dysregulation of stress hormones on the timescale of weeks. Molecular Systems Biology 2020; 16. DOI:10.15252/msb.20209510.
13 Cryan JF, O’riordan KJ, Cowan CSM, et al. The microbiota-gut-brain axis. Physiol Rev 2019; 99: 1877–2013.
14 Zhang QE, Wang F, Geng Q, et al. Depressive symptoms in patients with irritable bowel syndrome: A meta-analysis of comparative studies. International Journal of Biological Sciences 2018; 14: 1504–12.
15 Safadi JM, Quinton AMG, Lennox BR, Burnet PWJ, Minichino A. Gut dysbiosis in severe mental illness and chronic fatigue: a novel trans-diagnostic construct? A systematic review and meta-analysis. Molecular Psychiatry 2021; : 1–13.
16 Scheri GC, Fard SN, Schietroma I, et al. Modulation of tryptophan/serotonin pathway by probiotic supplementation in human immunodeficiency virus-positive patients: Preliminary results of a new study approach. International Journal of Tryptophan Research 2017; 10. DOI:10.1177/1178646917710668.
17 Messaoudi M, Lalonde R, Violle N, et al. Assessment of psychotropic-like properties of a probiotic formulation (Lactobacillus helveticus R0052 and Bifidobacterium longum R0175) in rats and human subjects. British Journal of Nutrition 2011; 105: 755–64.
18 Milajerdi A, Mousavi SM, Sadeghi A, et al. The effect of probiotics on inflammatory biomarkers: a meta-analysis of randomized clinical trials. European Journal of Nutrition 2020; 59: 633–49.
19 Silva YP, Bernardi A, Frozza RL. The Role of Short-Chain Fatty Acids From Gut Microbiota in Gut-Brain Communication. Frontiers in Endocrinology 2020; 11: 25.
20 Wu M, Tian T, Mao Q, et al. Associations between disordered gut microbiota and changes of neurotransmitters and short-chain fatty acids in depressed mice. Translational Psychiatry 2020; 10: 1–10.
21 Wallace CJK, Milev R. The effects of probiotics on depressive symptoms in humans: A systematic review. Annals of General Psychiatry 2017; 16: 14.
22 Bron PA, Kleerebezem M, Brummer RJ, et al. Can probiotics modulate human disease by impacting intestinal barrier function? British Journal of Nutrition 2017; 117: 93–107.
23 Dinan TG, Cryan JF. Microbes Immunity and Behavior: Psychoneuroimmunology Meets the Microbiome. Neuropsychopharmacology 2017; 42: 178–92.


